WELCOME TO OUR PARKINSON'S PLACE!
I HAVE PARKINSON'S DISEASES AND THOUGHT IT WOULD BE NICE TO HAVE A PLACE WHERE THE CONTENTS OF UPDATED NEWS IS FOUND IN ONE PLACE. THAT IS WHY I BEGAN THIS BLOG.
I COPY NEWS ARTICLES PERTAINING TO RESEARCH, NEWS AND INFORMATION FOR PARKINSON'S DISEASE, DEMENTIA, THE BRAIN, DEPRESSION AND PARKINSON'S WITH DYSTONIA. I ALSO POST ABOUT FUNDRAISING FOR PARKINSON'S DISEASE AND EVENTS. I TRY TO BE UP-TO-DATE AS POSSIBLE.
I AM NOT RESPONSIBLE FOR IT'S CONTENTS. I AM JUST A COPIER OF INFORMATION SEARCHED ON THE COMPUTER. PLEASE UNDERSTAND THE COPIES ARE JUST THAT, COPIES AND AT TIMES, I AM UNABLE TO ENLARGE THE WORDING OR KEEP IT UNIFORMED AS I WISH. IT IS IMPORTANT TO UNDERSTAND I AM A PERSON WITH PARKINSON'S DISEASE. I HAVE NO MEDICAL EDUCATION,
I JUST WANT TO SHARE WITH YOU WHAT I READ ON THE INTERNET. IT IS UP TO YOU TO DECIDE WHETHER TO READ IT AND TALK IT OVER WITH YOUR DOCTOR. I AM JUST THE COPIER OF DOCUMENTS FROM THE COMPUTER. I DO NOT HAVE PROOF OF FACT OR FICTION OF THE ARTICLE. I ALSO TRY TO PLACE A LINK AT THE BOTTOM OF EACH ARTICLE TO SHOW WHERE I RECEIVED THE INFORMATION SO THAT YOU MAY WANT TO VISIT THEIR SITE.
THIS IS FOR YOU TO READ AND TO ALWAYS KEEP AN OPEN MIND.
PLEASE DISCUSS THIS WITH YOUR DOCTOR, SHOULD YOU HAVE ANY QUESTIONS, OR CONCERNS. NEVER DO ANYTHING WITHOUT TALKING TO YOUR DOCTOR FIRST..
I DO NOT MAKE ANY MONEY FROM THIS WEBSITE. I VOLUNTEER MY TIME TO HELP ALL OF US TO BE INFORMED.
I WILL NOT ACCEPT ANY ADVERTISEMENT OR HEALING POWERS, HEALING FROM HERBS AND ETC. UNLESS IT HAS GONE THROUGH TRIALS AND APPROVED BY FDA. IT WILL GO INTO SPAM.
THIS IS A FREE SITE FOR ALL WITH NO ADVERTISEMENTS
THANK YOU FOR VISITING! TOGETHER WE CAN MAKE A DIFFERENCE!
TRANSLATE
Tuesday, August 9, 2011
What is Deep Brain Stimulation for Parkinson's Disease?
9th August 2011; THE LONG TERM EFFECTS OF DBS ON PARKINSON'S DISEASE
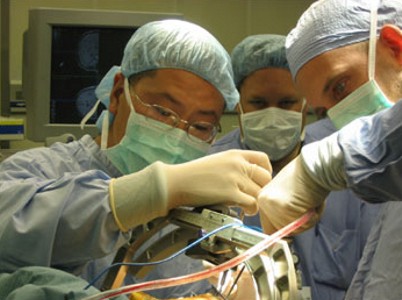 DBS improved the Parkinson's Disease symptom score by 25% in comparison to no treatment, including resting and action tremor by over 85%, and bradykinesia by 23%. It did not stop deterioration in speech, walking, and postural instability, including falling and freezing. L-dopa dosages reduced to about 63% of what they were initially. Daily living activity also improved. Dyskinesia and motor fluctuation scores also remained significantly lower. Potential adverse events included : a trend to weight loss, visual hallucinations, impulse control disorders possibly related to dopamine agonists, progressive cognitive decline culminating in dementia, device related infections.
DBS improved the Parkinson's Disease symptom score by 25% in comparison to no treatment, including resting and action tremor by over 85%, and bradykinesia by 23%. It did not stop deterioration in speech, walking, and postural instability, including falling and freezing. L-dopa dosages reduced to about 63% of what they were initially. Daily living activity also improved. Dyskinesia and motor fluctuation scores also remained significantly lower. Potential adverse events included : a trend to weight loss, visual hallucinations, impulse control disorders possibly related to dopamine agonists, progressive cognitive decline culminating in dementia, device related infections. Monday, August 8, 2011
Nicotine Protects Against Parkinson’s?
Northwest Parkinson's Foundation:
 The addictive component of cigarettes saves dopamine neurons from a Parkinson’s-like decline, providing a new avenue for potential treatment.Jef Akst
The addictive component of cigarettes saves dopamine neurons from a Parkinson’s-like decline, providing a new avenue for potential treatment.Jef AkstBy activating the alpha-7 nicotinic receptor, nicotine—which increases dopamine levels in the brain—appears to be able to rescue mouse dopaminergic neurons cultured under conditions that favor their loss. Genetically engineered mouse cells that lacked a specific nicotine receptor (the alpha-7 subtype), however, were unaffected by nicotine treatment.
The findings suggest that new Parkinson’s therapies may be developed to target nicotine receptors, FierceBiotech reports. “This study raises the hope for a possible neuroprotective treatment,” said co-author Patrick P. Michel of the Institut du Cerveau et de la Moelle Épinière, Hôpital de la Salpêtrière, in Paris, France, in a statement.
But this is not an endorsement for cigarettes, FASEB noted. “If you’re a smoker, don’t get too excited,” Gerald Weissmann, editor-in-chief of The FASEB Journal, said in a statement. “Even if smoking protects you from Parkinson’s, you might not live long enough to develop the disease because smoking greatly increases the risk for deadly cancers and cardiovascular diseases.”
Sleep Disorder is Risk Factor for Parkinson’s
From the Northwest Parkinson's Foundation: Rick Nauert PhD
 Psych Central - A new European study suggests individuals suffering from REM sleep behavior disorders have an increased risk of developing Parkinson’s disease (PD).
Psych Central - A new European study suggests individuals suffering from REM sleep behavior disorders have an increased risk of developing Parkinson’s disease (PD).REM sleep behavior disorders are characterized by dream nightmares in which a person is attacked and pursued leading an individual to scream, cry, punch and kick while sleeping.
The current study is the third work on the topic within the last five years to be published by Lancet Neurology.
The first work showed in 2006 that 45 percent of patients who suffer this sleep disorder develop Parkinson’s disease and other neurodegenerative diseases caused by a lack of dopamine in the brain.
The second article discovered that neuroimaging tests that measure dopamine in the brain, such as the brain SPECT scan (single-photon emission computed tomography), are useful to identify patients with REM sleep disorders with increased risk of developing a neurodegenerative diseases such as Parkinson’s disease.
In the current study, researchers used SPECT to conclude that the levels of dopamine in the brain are quickly lowering over the years in patients with REM sleep behavior disorder.
SPECT is the first neuroimaging technique to detect the disease progression at an early stage. The study involved comparing for three years the evolution of brain SPECT in 20 patients with REM disorder and 20 healthy controls.
The neuroimaging technique measures the presence of dopamine in the substantia nigra, a part of the brain associated with learning and harmony of body movements. In Parkinson’s disease, a deficiency of dopamine in the substantia nigra causes tremor, stiffness and movement slowness in patients.
Results showed that after three years of monitoring the production of dopamine in the control group was reduced by 8 percent due to age, while the group of REM sleep disorder patients experienced a reduction of 20 percent.
Once the three-year follow-up ended, three of 20 patients in the REM sleep disorder group had developed Parkinson’s disease and their dopamine reduction was around 30 percent.
Researchers conclude that more efforts are needed to create neuroprotective drugs that prevent the progression from REM sleep behavior disorders to Parkinson’s disease.
Authors of the study suggest that, to be considered effective, a neuroprotective drug should significantly prevent the dopamine concentration from dropping in these patients.
