Ideggyogy Sz. [2013] 66 (3-4) : 115-120 (G.Tamás, A.Takáts, P.Radics, I.Rózsa, E.Csibri, G.Rudas, P.Golopencza, L.Entz, D.Fabó, L.Eross)
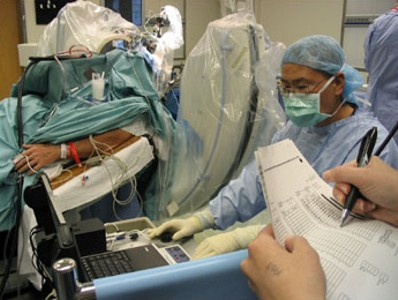 The major Parkinson's Disease symptom score (the Unified Parkinson's Disease Rating Scale) decreased by 70%. Patient condition improved according to the Hoehn-Yahr scale, approximately by two stages. Twelve hours after the withdrawal of Parkinson's Disease drugs execution of daily activity improved by 57% and motor functions developed by 79%. Duration of dyskinesias decreased by 62%. Duration of akinesia (loss of movement) diminished by 87%. Quality of life rose by 41%. Neuropsychological tests detected improvement in verbal memory. The dosage of Parkinson's Disease drugs could be reduced by 63% after the operation had been completed.
The major Parkinson's Disease symptom score (the Unified Parkinson's Disease Rating Scale) decreased by 70%. Patient condition improved according to the Hoehn-Yahr scale, approximately by two stages. Twelve hours after the withdrawal of Parkinson's Disease drugs execution of daily activity improved by 57% and motor functions developed by 79%. Duration of dyskinesias decreased by 62%. Duration of akinesia (loss of movement) diminished by 87%. Quality of life rose by 41%. Neuropsychological tests detected improvement in verbal memory. The dosage of Parkinson's Disease drugs could be reduced by 63% after the operation had been completed.They concluded that, with Deep Brain Stimulation and by careful patient selection, the dosage of Parkinson's Disease drugs could be significantly reduced with considerable improvements in motor function and quality of life.